Diabetes is a national epidemic. According to the Centers for Disease Control, 31 million Americans are living with diabetes, Also, 85 million Americans have pre-diabetes that can lead to full-blown diabetes.
Diabetic foot wounds and pain are a complication of diabetes. Therefore, it is important for diabetics to have good quality foot care. In order for diabetics to protect their feet, they must have a good diabetic shoe. The pain is from peripheral neuropathy. In this article, learn about the best diabetic neuropathy wounds and foot pain solutions.
The Best Diabetic And Foot Pain Solutions
It is estimated that between 65% -70% of people with diabetes have neuropathy. Diabetic neuropathy is a common disorder found in diabetic persons.
Diabetic neuropathy is a peripheral nerve dysfunction that causes pain and numbness in extremities, mainly the legs. Neuropathy can occur in any part of the body, but it mainly occurs in the feet. Revitanerve supplement is helpful in easing diabetic foot pain.
Diabetic Foot Care
It is important to wear diabetic shoes that are comfortable and that have velcro closures. Velcro closures make it easier to adjust on the feet. Diabetics must also wear diabetic socks at all times so the feet do not sweat. Wet feet will make the feet more susceptible to break down.
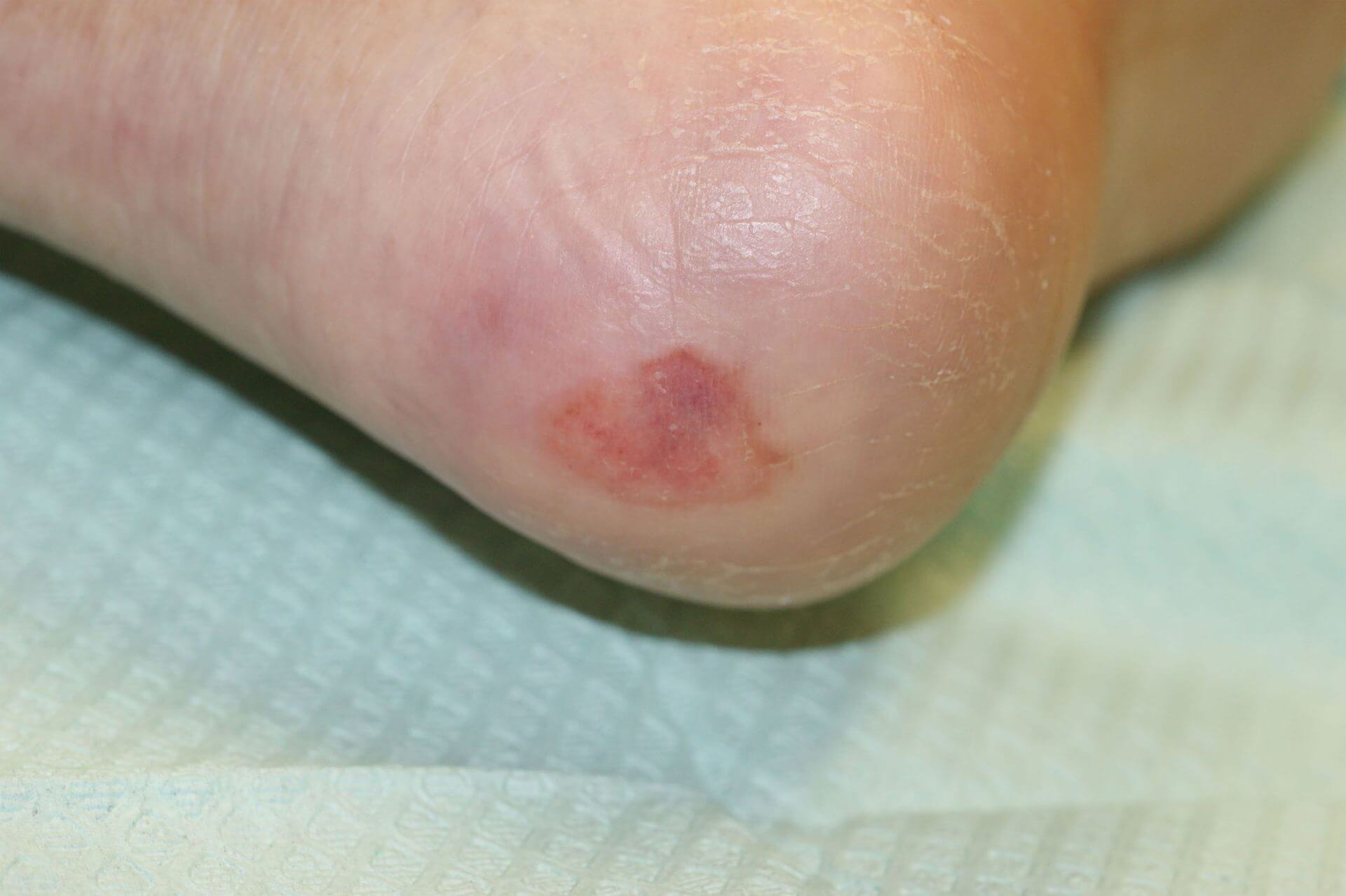
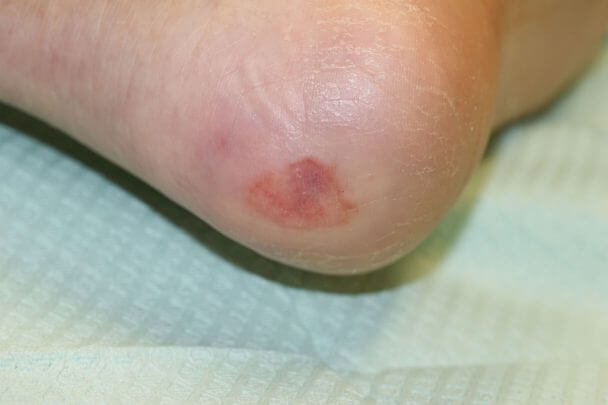
Diabetic foot wounds are a major cause of disability. These foot wounds often lead to hospitalizations for infections and amputations. Diabetic wounds are complicated by neuropathy, infection, and ischemia.
Diabetic foot ulcers are extremely common. It is estimated that 20% of all diabetic patients will have a diabetic foot wound. Of those wounds, 15% will go on to have an amputation.
How to Avoid Diabetic Foot Wounds
- A diabetic should check their feet every day for cuts, bruises, swelling, and sores.
- Callouses and corns should be evaluated by a podiatrist. O’Keeffe’s foot cream is a highly rated cream that heals and repairs dry, cracked feet. This cream creates a protective layer on the skin’s surface that instantly boosts moisture levels and helps prevent further moisture loss.
- A diabetic should wash their feet every day. This tea tree oil is excellent to clear the feet of fungus and any other irritants. Don’t soak your feet. Do not apply lotion between your ties because it can lead to infection.
- Always wear shoes on your feet. Propet Men’s Sneaker or the Propet Women’s Sneaker are excellent options for a diabetic’s feet.
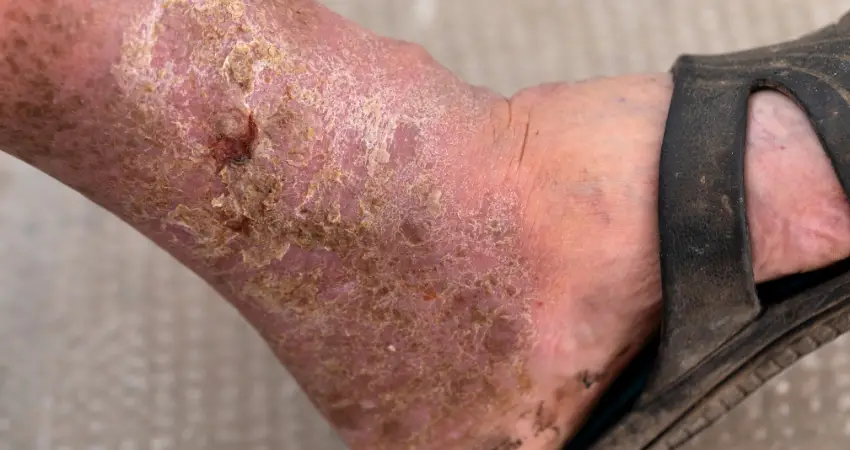
Signs of Foot Problems in the Diabetic
- Pain in your lower extremities or cramping in your thighs, legs, or calves during physical activity
- Tingling, numbness or burning in your feet
- A change in the shape of your feet over time
- Hair loss on your toes, feet, and lower legs
- Dry and cracked skin on your feet
- A change in the color and temperature of your feet
- Thick, yellow or brown toenails
- Blisters, sores, ulcers, infected corns, or ingrown toenails
- Fungus infections such as athlete’s foot between your toes
Related Articles
Pictures of Swollen Ankles Due to Congestive Heart Failure
Gifts for Stroke Survivors
Stroke and Afib With tPA
What Causes Foot Ulcers?
Diabetic foot ulcers are caused by neuropathy, ischemia, and peripheral vascular disease. Diabetes causes damage to the nerves of the foot.
This produces foot deformities that lead to bony prominence. This will eventually lead to skin breakdown on the feet.
Nerve damage causes the feet to not sweat as much. Therefore, the skin will become dry and cracked, and develop an infection.
The diabetic person needs to make sure that they keep their feet clean and moist with a cream such as Neoteric Diabetic.
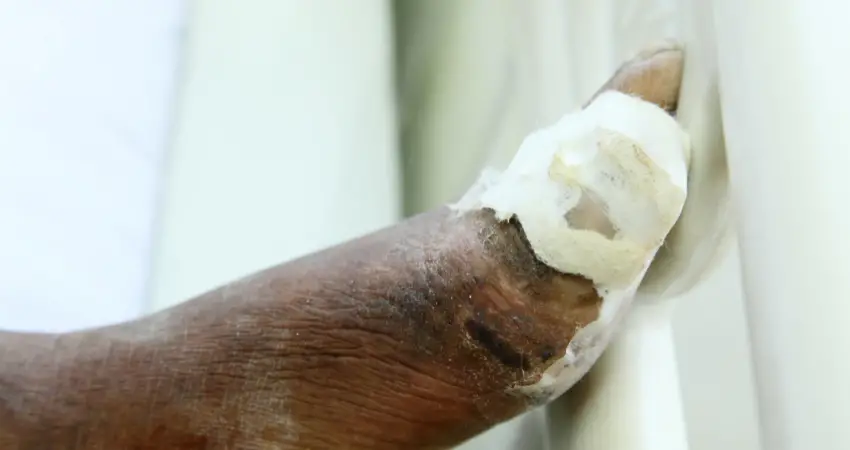
When a diabetic has nerve damage, they lose sensation in their feet. As a result, when a diabetic has trauma to their feet, often time they cannot feel the trauma.
For example, diabetics will often get burns in the shower because they are unable to feel the hot temperature.
Many of these people will get third-degree burns. Also, some people will walk barefoot on the hot sidewalk, and they will get third-degree burns.
These burns are extremely hard to heal because the foot already has nerve damage, which means the vessels to the foot are also probably damaged.
Therefore, blood and nutrients cannot get to the foot and provide proper healing. For small burns, Vitastem is a great cream for burns.
Often, many wounds go unnoticed because the person simply cannot feel them.
These wounds continue to get worse and worse because the diabetic continues to walk on the wound and put pressure on the wound.
Diabetes Foot Complications
Charcot arthropathy is a result of peripheral neuropathy. This disorder leads to change in the arches of the feet, which leads to the bone losing minerals.
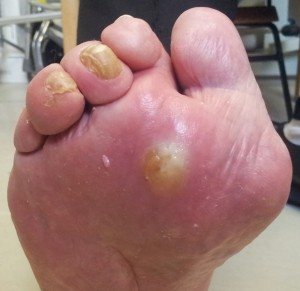
Osteomyelitis
Osteomyelitis results from a deep tissue infection that goes to the bone marrow. A large percentage of foot wounds end up as osteomyelitis. Diagnosing osteomyelitis in a patient with a diabetic foot is often difficult. Major problems include differentiating soft tissue infection from bone infection and infections from non-infectious disorders (Charcot Foot).
How to Examine the Feet
Examination of the feet is an important part of the exam for a diabetic patient. A diabetic should be checking their feet for dry skin, open sores, fissures, ulcers, big veins, and hair loss. Check the bottom of the foot for bony points. The foot should also be examined for hotness or cold temperature. The pulses in the foot should be able to be palpated.
If no pulse can be felt, the diabetic should go to a doctor as soon as possible to get a doppler check done. The newer imaging techniques are nuclear bone scan, computerized tomography scan (CT), positron emission tomography (PET), and magnetic resonance imaging (MRI). Of these, MRI is more sensitive and specific.
“The management of diabetic foot ulcers includes several facets of care. Offloading and debridement are considered vital to the healing process, for diabetic foot wounds. The goal of offloading is to redistribute force from the ulcers sites and pressure points at risk, to a wider area of contact. There are multiple methods of pressure relief, including total contact casting, half shoes, removable cast walkers, wheelchairs, and crutches.”
Bottom Line:
Prevention of diabetic foot includes:
-
Primary prevention: Screening of high-risk feet and proper advice on preventive footwear
-
Secondary prevention: Management of trivial foot lesions such as callus removal, treatment of nail pathologies, deroofing blisters, and so on.
-
Tertiary prevention: Prompt referral to a specialist for advanced foot lesions
References:
.
My name is Phyllis Robinson MSN, RN. I have been a Registered Nurse for 27 years in the Cardiac Intensive Care Unit. I am passionate about cardiac care and heart disease. I also want this blog to be an educational tool that people can refer to for traditional and alternative treatment. I will blog on heart disorders such as high blood pressure, congestive heart failure, cardiomyopathy, and high cholesterol.
I received my Nursing degree from Baltimore Community College.
I went on to receive my Masters in Nursing from Walden University
I have worked for almost 30 years in Critical Care with a focus on heart health. I am an advocate of preventive healthcare.