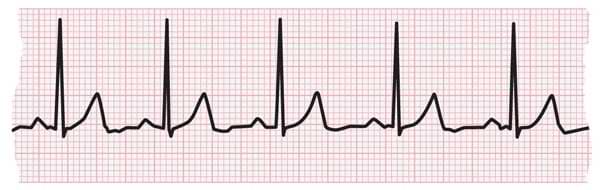
What is an EKG?
An electrocardiogram (EKG or ECG) is a non-invasive, diagnostic test that measures the electrical activity of the heart. It’s used to assess the heart’s rhythm and the conduction of electrical impulses through the heart muscle. This is typically done by placing electrodes on the patient’s chest, arms, and legs.
What is it looking for?
An EKG is looking for a variety of things related to the heart’s function. It can detect and record many types of heart problems, including:
- Arrhythmias, or abnormal heart rhythms.
- Coronary artery disease, which can cause inadequate blood flow to the heart.
- Previous heart attacks, shown by damage to the heart muscle.
- Ongoing heart attacks, by showing areas of the heart muscle that aren’t receiving enough oxygen.
- Problems with the electrical conduction system of the heart.
- Cardiomyopathy, or thickening of the heart muscle.
- Other structural abnormalities, such as an enlarged heart.
What are the limitations of the EKG?
While an EKG is a valuable diagnostic tool, it does have limitations:
- It only represents a snapshot in time: Heart conditions that are intermittent may not be detected unless they happen while the EKG is being done.
- It’s not definitive for all heart diseases: Some heart conditions may not affect the electrical conduction of the heart, and therefore may not be detected by an EKG.
- EKG doesn’t provide a direct measurement of heart function: An EKG cannot provide a direct assessment of how well the heart is pumping, or the condition of the heart valves.
- EKG doesn’t show blockages: An EKG cannot show the presence of coronary artery blockages unless the blockage is causing a current or past heart attack.
What will happen if a patient has a positive EKG?
A “positive” EKG typically means the test has detected some abnormality in the heart’s electrical activity. Depending on the specific findings, different actions may be taken:
- Further diagnostic testing: If an EKG suggests a heart condition, further tests, such as an echocardiogram, stress test, or angiogram, may be ordered to gather more information.
- Treatment: If the EKG shows an ongoing heart attack, immediate treatment is necessary to restore blood flow to the heart muscle. This might involve medication, a procedure to open the blocked artery, or surgery.
- Monitor and follow-up: If the EKG shows a less urgent issue, such as a minor arrhythmia or non-critical heart condition, the patient may be monitored and scheduled for a follow-up appointment.
- Medication adjustments: If the EKG shows that a current medication is causing heart problems, such as an arrhythmia, the medication may be adjusted or stopped.
The specifics will depend greatly on the patient’s individual health, the exact findings of the EKG, and the judgment of their healthcare provider.
Conclusion
In conclusion, an Electrocardiogram (EKG or ECG) is a crucial diagnostic tool in medicine used to evaluate the electrical activity within the heart. This test provides invaluable insights into a variety of heart conditions such as arrhythmias, coronary artery disease, heart attacks, problems with the heart’s electrical conduction system, cardiomyopathy, and other structural abnormalities.
However, it’s essential to understand that EKGs have limitations. They provide a snapshot of the heart’s activity at the time of the test, which may miss intermittent issues. They aren’t definitive for all heart conditions, and they can’t provide direct measurements of heart function or the presence of coronary artery blockages.
A positive EKG indicates some abnormality in the heart’s electrical activity. The subsequent actions depend on the specific findings but may include further diagnostic tests, immediate treatment, monitoring and follow-ups, or medication adjustments.
Given these considerations, while EKGs are a vital part of diagnosing and managing heart disease, they are most effective when used in conjunction with a patient’s full medical history, physical examination, and other diagnostic tests as deemed necessary by a healthcare professional.
FAQ
What is an EKG?
An EKG, or electrocardiogram, is a test that records the electrical activity of your heart. It is a non-invasive test that is painless and takes only a few minutes to perform.
What does an EKG measure?
An EKG measures the electrical activity of your heart. The electrical activity of your heart is generated by the heart’s own pacemaker, which is a group of cells located in the upper right chamber of your heart. The electrical activity travels through the heart’s chambers, causing them to contract and pump blood.
What can an EKG tell you?
An EKG can tell you a lot about your heart’s health. It can be used to diagnose a variety of heart conditions, including:
- Heart attack
- Arrhythmia
- Heart failure
- Heart muscle damage
- Heart valve problems
An EKG can also be used to monitor your heart’s health over time. If you have a history of heart problems, your doctor may order an EKG on a regular basis to check for any changes in your heart’s electrical activity.
How is an EKG performed?
An EKG is performed by a technician who will place 12 electrodes on your chest, arms, and legs. The electrodes are connected to an EKG machine, which records the electrical activity of your heart.
The technician will ask you to lie still on a table while the EKG is being performed. The test is painless and takes only a few minutes to complete.
What should I expect after an EKG?
After the EKG is complete, you can go about your normal activities. There is no special care required after an EKG.
What are the risks of an EKG?
There are no risks associated with an EKG. It is a safe and painless test.
What are the benefits of an EKG?
An EKG can be a valuable tool for diagnosing and monitoring heart problems. It is a quick, easy, and painless test that can help your doctor to assess your heart’s health.
How far back can an EKG detect a heart attack?
An electrocardiogram (EKG or ECG) is a diagnostic test that measures the electrical activity of the heart. It is commonly used to assess the heart’s rhythm and detect various abnormalities, including signs of a heart attack. However, the time frame in which an EKG can detect a heart attack depends on several factors:
- Time of occurrence: An EKG is most effective at detecting a heart attack when it is performed during or shortly after the episode. The electrical changes associated with a heart attack can be detected on an EKG immediately after the onset of symptoms, such as chest pain or discomfort.
- Extent of damage: The EKG’s ability to detect a heart attack also depends on the extent of damage to the heart muscle. If the heart attack is large and affects a significant portion of the heart, the changes on the EKG will be more pronounced and easier to identify.
- Type of heart attack: There are different types of heart attacks, including ST-segment elevation myocardial infarction (STEMI) and non-ST-segment elevation myocardial infarction (NSTEMI). A STEMI involves complete blockage of a coronary artery, while an NSTEMI involves partial blockage. A STEMI is typically easier to detect on an EKG due to the distinctive changes it produces.
In general, an EKG can detect a heart attack as soon as the characteristic changes in the heart’s electrical activity occur. These changes can be visible within minutes of the onset of a heart attack. However, it’s worth noting that in some cases, an EKG may fail to detect a heart attack if the changes are subtle or if the test is performed too long after the event.
If there is a suspicion of a heart attack, it is important to seek immediate medical attention. A healthcare professional will consider various factors, including the patient’s symptoms, medical history, and other diagnostic tests, in addition to the EKG results, to make an accurate diagnosis and determine the appropriate course of treatment.